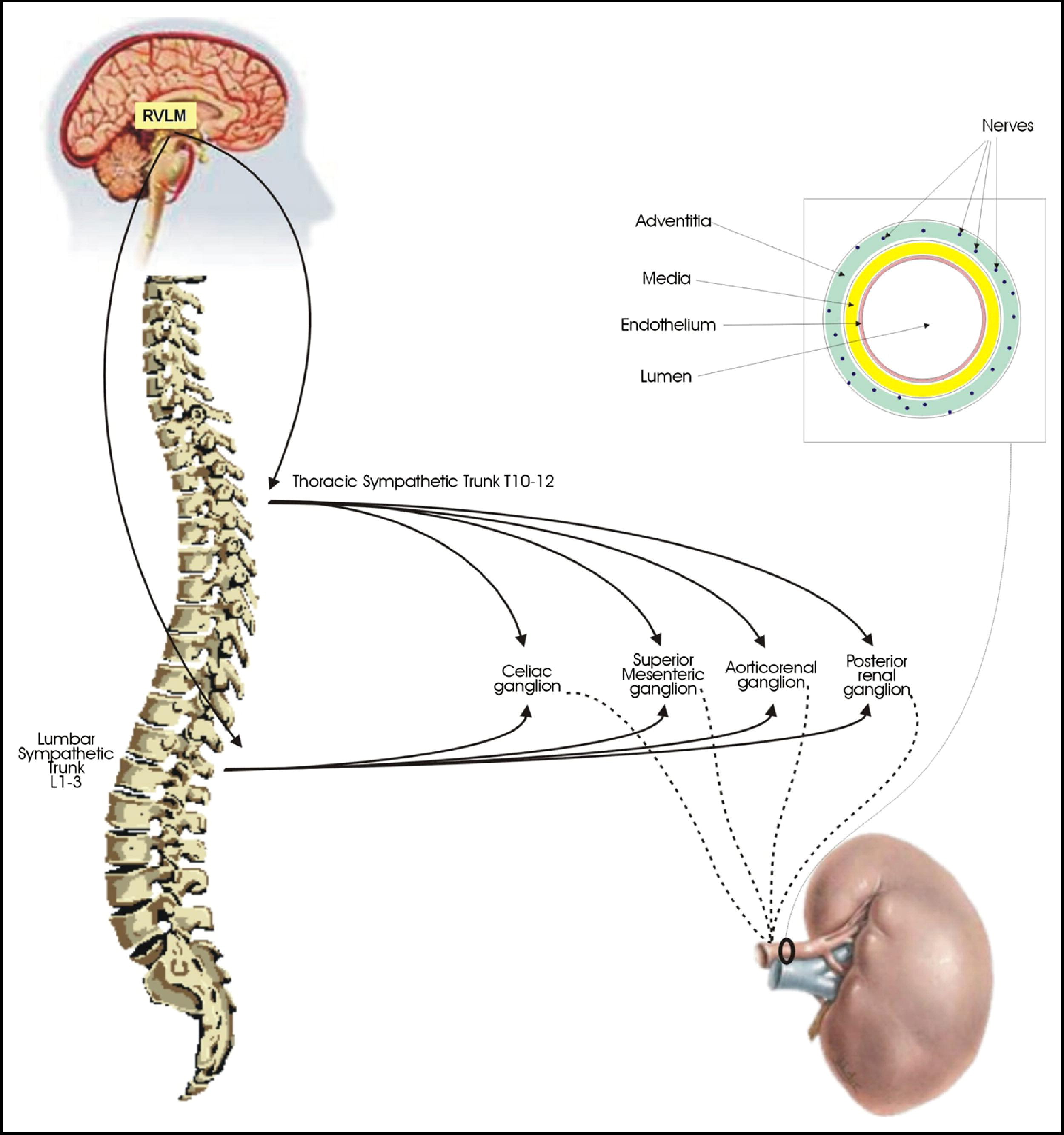
Renal Sympathetic Denervation - Current And Future Trends
Catheter-based renal sympathetic denervation therapy is an interesting and promising new therapeutic method that has the potential to change the present treatment paradigm in patients.
Author:Karan EmeryReviewer:James PierceAug 03, 20238.7K Shares335.7K Views
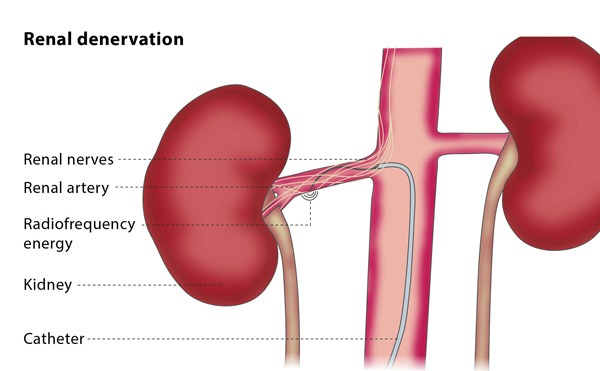
High blood pressure that has not responded to therapy is resistant hypertension. Renal sympathetic denervationis a minimally invasive treatment used to treat resistant hypertension.
Radiofrequency ablation is used to burn the nerves in the renal arteries. This mechanism induces a decrease in nerve activity, which lowers blood pressure.
Catheter-based renal sympathetic denervation therapy is an exciting and promising new therapeutic method that has the potential to change the present treatment paradigm in patients.
Renal Denervation For Resistant Hypertension
Resistant hypertension is characterized as blood pressure that remains raised over 140/90 mmHg despite lifestyle changes (e.g., exercise/salt restriction, among others) and using three or more antihypertensive medications.
Resistant hypertension is estimated to affect 12% of persons diagnosed with hypertension in the United States or around 9 million people. Patients with resistant hypertension have a much increased cardiovascular risk, with a 50% increase in major events compared to persons with regulated blood pressure.
To date, the role of the renal sympathetic nervous system in controlling blood pressure and other autonomic processes was unknown. In animal investigations, invasive renal sympathetic denervation was shown to diminish afferent and efferent sympathetic activity, essential in developing hypertension, heart failure, and renal disease.
Renal Denervation History
Renal denervation goes back to 1953 when splanchnicectomy (surgical removal of renal nerves) was mentioned as a therapy option in individuals with severe primary hypertension. Interventional radiofrequency methods were developed in the 1990s, and proof-of-concept trials revealed considerable decreases in blood pressure following renal denervation.
The renal denervation technique was carried out in the catheterization lab using either radiofrequency energy, ultrasound energy, or neurotoxic chemicals (alcohol), with no clear indication that one way is preferable.
Renal Sympathetic Denervation Devices
Symplicity
The most significant clinical experience has been gained with the Symplicity (Medtronic Inc., CA, USA) catheter, which is designed to transport radiofrequency radiation through the renal artery wall to achieve renal denervation. It is currently the only commercially available gadget having clinical usage data from randomized controlled studies.
Before operating on the contralateral artery, 2 minutes of radiological energy alternating at radiofrequency is supplied and repeated four to six times in a helical pattern. The total treatment time would be 24 minutes if each side got six sessions. A brief study found that renal denervation with the Symplicity catheter had a great safety profile and led to a significant and sustained office BP decrease of 27/17 mmHg after 12 months.
Symplicity HTN-2 is the largest prospective, randomized trial ever conducted. This study included 106 participants who were randomly allocated to either renal denervation or a control group, using the same inclusion criteria as the prior experiment.
The Symplicity HTN-3 study is a randomized, single-blind study that compares renal denervation to a sham procedure. Its enrollment is complete, and the preliminary results are expected in 2014. Changes in office systolic blood pressure from baseline to 6 months and severe adverse events from baseline to 1 month are the primary objectives.
Despite no safety problems, Symplicity HTN-3 did not fulfill its critical efficacy end goal, according to a recent news release from Medtronic, Inc.
The EnligHTN System
Four companies that manufacture renal denervation devices have earned the EU CE mark: EnligHTNTM (St Jude Medical, MN, USA), VessixTM Vascular V2 (Boston Scientific, MA, USA), OneShotTM (Covidien, CA, USA), and PARADISE® are all products of St Jude Medical (ReCor Medical, CA, USA).
Despite the lack of evidence from randomized trials for any of these devices, preliminary first-in-human studies have shown promise. Although the six-month decline in in-office blood pressure is similar to that reported in the early Symplicity trials, these studies also included ambulatory blood pressure data, though formal reporting is still awaiting.
EnligHTN is an 8 F-compatible device comprising four monopolar electrodes on an extendable basket with a deflectable tip connected to a radiofrequency generator. A typical dispersive electrode is applied to the skin (grounding pad).
The EnligHTN I study looked at the safety and blood pressure reduction of 46 persons who had an office systolic blood pressure of 160 mmHg (or 150 mmHg if they had diabetes) and were using three or more antihypertensive medications. At six months, the average drop in-office blood pressure was 26/10 mmHg.
The OneShot System
The OneShot Device is a 9 F-compatible balloon-mounted apparatus with a helical silver monopolar electrode connected to a radiofrequency generator. The balloon is inflated to nominal size with normal saline at 1 Atm pressure during ablation, and saline seeps through micropores, rinsing, cooling, and limiting harm to non-target tissue.
Treatment time is typically 2 minutes on each side. An early feasibility study of nine patients at 12 months demonstrated a 31/10 mmHg drop-in office BP. A randomized controlled study is now underway.
System Vessix V2
The Vessix V2 is a balloon-delivered device with bipolar radiofrequency electrodes inserted in a helical pattern on the balloon. At the same time, all electrodes provide energy. Ablative energy is typically delivered in 30 seconds on each side, resulting in a quicker process than the Symplicity system. The early results of a 120-patient feasibility study revealed a 27/12 mmHg drop-in office BP after six months.
Renal Sympathetic Denervation Devices Future Prospects
The Symplicity Spyral Multi-Electrode Renal Denervation Catheter (Medtronic, Inc.) uses four electrodes to administer radiofrequency radiation via a highly conformable catheter. TIVUS (Cardiosonic, Tel Aviv, Israel) is a preclinical ultrasound device that employs endoluminal high-intensity ultrasound. Low-intensity focused ultrasound directed from an external source is used by the Kona Medical System (Campbell, California, USA).
Typical electrophysiological microcatheters for renal denervation therapies have also been studied. Theoretical advantages of adopting this technology include concerns that heat generated at the tissue-electrode interface during radiofrequency energy delivery may induce surface injury but limit the depth of the lesion while causing a nidus for char formation on the catheter. ThermoCool (Biosense Webster, CA, USA) and Mariner (Medtronic, Inc.) evaluated devices and found them effective.
Another method for generating renal denervation is to inject autonomic nerve blockers locally. The Bullfrog Microinfusion catheter (Mercator MedSystems, Inc., CA, USA) is a microneedle catheter with a balloon sheath. After the balloon has been stabilized by saline inflation, guanethidine is delivered through the microneedle to provide localized sympathectomy. Early studies in pig models demonstrated that medicine was administered effectively and that renal norepinephrine production was significantly reduced.
Other novel device technologies are being developed, and existing catheter systems are being updated. Many systems are expected to become 6 F guide-compatible and capable of reaching the renal arteries through a radial approach in the near future, reducing vascular access site-related complications. Noninvasive denervation methods, such as externally delivered ultrasound may also be accessible.
Advantages Of Renal Sympathetic Denervation
Aside from hypertension, increased sympathetic activity is linked to various other diseases. While hypothetical and untested, renal sympathetic denervation may be therapeutic in treating diabetes, heart failure, chronic renal disease, and arrhythmias.
Glucose Management
Sympathetic nerve activity is essential in developing insulin resistance and diabetes. Recent brief research investigated the impact of renal sympathetic denervation on glucose metabolism in patients with resistant hypertension.
Patients with treatment-resistant hypertension (n = 37) who got bilateral renal sympathetic denervation were compared to controls (n = 13). Those who received renal sympathetic denervation had significantly lower fasting glucose levels (118-108 mg/dl; p = 0.039) and basal insulin requirements (20.8 3.0 to 9.3 2.5 IU/ml; p = 0.006) after 3 months of follow-up. Similarly, 10 people with resistant hypertension and obstructive sleep apnea improved their glucose tolerance following renal sympathetic denervation.
Heart Arrhythmias
Renal sympathetic denervation may benefit arrhythmia treatment because autonomic tone influences chronotropy, dromotropy, the sinus node, and atrioventricular conduction. In humans, renal sympathetic denervation has been shown to reduce heart rate while increasing PR interval.
In animal tests, renal sympathetic denervation was shown to improve rate control and lower the incidence of atrial fibrillation. In a recent small-scale hypothesis-generating study, 27 patients with atrial fibrillation and hypertension undergoing pulmonary vein isolation were randomly randomized to either renal sympathetic denervation (n = 13) or a control (n = 14).
Individuals who had both pulmonary vein isolation and renal sympathetic denervation had a significantly lower chance of recurrence of atrial fibrillation at 12 months. Renal sympathetic denervation has also been utilized successfully to treat ventricular tachyarrhythmia storm in two patients with nonobstructive hypertrophic and dilated cardiomyopathy.
After renal sympathetic denervation, both subjects' ventricular tachyarrhythmia frequency improved dramatically. Before drawing firm conclusions, more experience in both contexts is essential.
Cardiovascular Disease
Pharmacological betablockade has been shown to reduce cardiovascular morbidity and death in systolic heart failure, most likely through regulating sympathetic nerve activity. A recent study on renal sympathetic denervation in this scenario suggests that it may improve symptoms and exercise tolerance after 6 months.
Similarly, renal sympathetic denervation in individuals with resistant hypertension has been shown to reduce LV mass and improve diastolic dysfunction. This observation has given rise to the theory that renal sympathetic denervation may improve outcomes in heart failure patients with a stable LV ejection fraction.
More study is being undertaken on the impact of renal sympathetic denervation in heart failure with adequate systolic function.
Unresolved Problems
Despite accumulating evidence that renal sympathetic denervation decreases blood pressure, no effect on morbidity or mortality has been demonstrated. No studies suggest that renal sympathetic denervation affects myocardial infarction, stroke, heart failure, renal failure, or death.
Some apparent benefits of renal sympathetic denervation might be attributable to a placebo effect. The 'alert reaction' and 'white-coat' effect may be more prominent during visit one due to the presence of a doctor in the consultation room. Other healthcare experts, on the other hand, may perform follow-up steps.
The primary end objective of safety comprises all-cause mortality, vascular complications, and procedure-related complications. There seems to be a nonresponse rate to renal sympathetic denervation between 10% and 30%. Methods for identifying whether a lack of reaction is caused by partial denervation may be necessary.
Mechanism Of Renal Denervation
The method by which renal sympathetic denervation improves blood pressure control is complicated, including the following factors:
- Reduced efferent sympathetic transmission to the kidneys
- Cutting down on norepinephrine overflow
- Natriuresis
- Enhancing renal blood flow
- Reduced plasma renin activity
- Reduced renal afferent signaling and sympathetic stimulation

Radiofrequency Renal Denervation Procedure
Renal Denervation Side Effects
Research and registries have shown that blood pressure drops consistently following renal denervation.
- hypertension.
- kidney function
- blood pressure systolic
- Chronic blood pressure, renal failure
- ambulatory blood pressure measurement
- follow-up.
- Hypertension of the kidneys
People Also Ask
Is Renal Denervation Permanent?
Renal denervation is permanent. Medication for the high blood pressure may be discontinued.
Is Renal Denervation Effective?
Renal denervation, a minimally invasive technique, is a potential new non-drug therapeutic option that may successfully manage blood pressure in people with resistant hypertension, according to growing research.
What Is Renal Sympathetic Nerve Activity?
Pathophysiological diseases such as hypertension and chronic and end-stage renal illness typically increase renal sympathetic nerve activity (RSNA). Increased RSNA elevates blood pressure and may lead to renal function impairment.
What Does Renal Denervation Do?
Renal denervation is a minimally invasive treatment used to treat resistant hypertension. Radiofrequency ablation is used to burn the nerves in the renal arteries. This technique reduces nerve activity, which lowers blood pressure.
Conclusion
Renal sympathetic denervation has the potential to be a beneficial adjunct to the best medical treatment for resistant hypertension. Due to various methodological shortcomings, the existing evidence is equivocal.
However, further study will help clarify the effectiveness of this approach. This might include cases when sympathetic nervous system overactivity is harmful, such as heart failure.

Karan Emery
Author

James Pierce
Reviewer
Latest Articles
Popular Articles