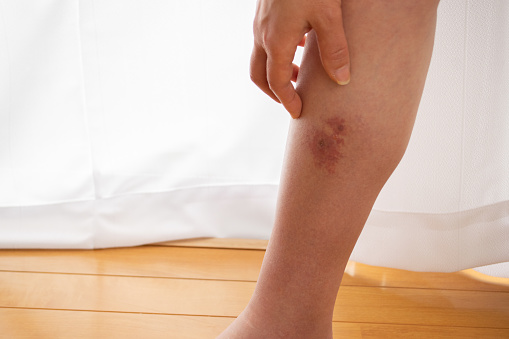
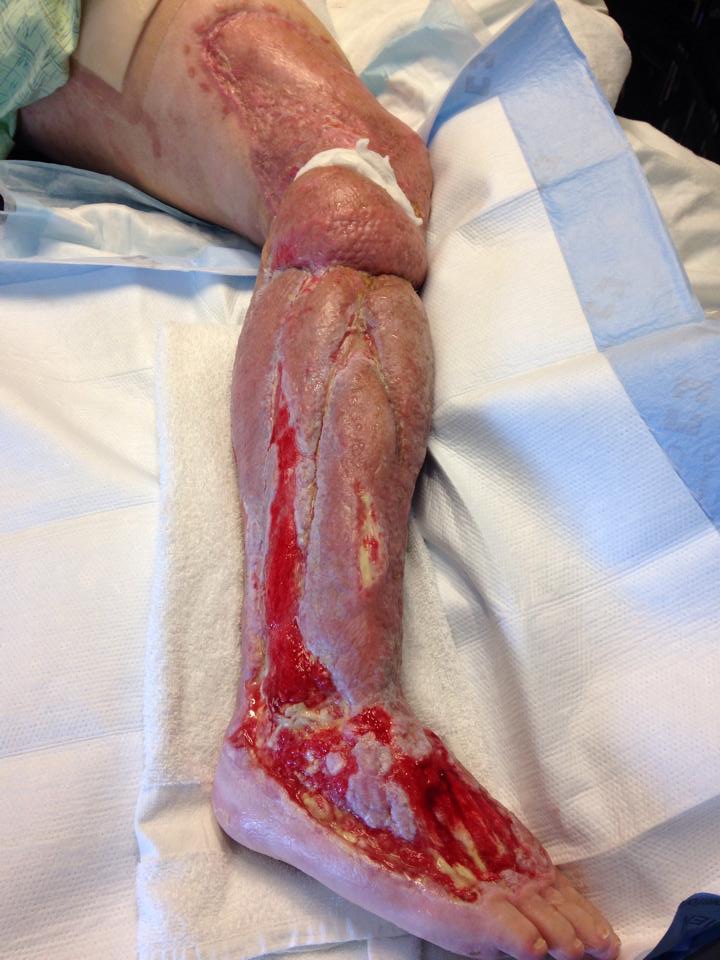
Necrotizing Fasciitis - The Cause, Symptoms And Treatment
Necrotizing fasciitis is a serious, uncommon, and sometimes fatal soft tissue infection affecting the scrotum, perineum, the abdominal wall, or the extremities.
Author:Katharine TateReviewer:Karan EmeryMay 27, 202357.1K Shares828.6K Views
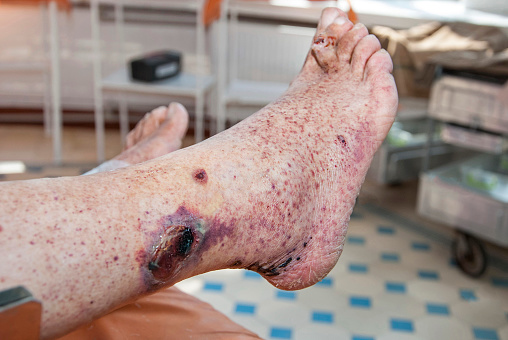
Necrotizing fasciitis(NF) is a serious, uncommon, and sometimes fatal soft tissue infection affecting the scrotum, perineum, the abdominal wall, or the extremities.
Co-morbidities like diabetes, immunosuppression, chronic alcohol illness, chronic renal failure, and liver cirrhosis worsen the prognosis.
Based on microbiological discoveries, necrotizing fasciitis is categorized into four kinds. The majority of cases are polymicrobial, classified as type I. The patient's clinical condition ranges from erythema, edema, and soreness in the early stages of infection to skin ischemia with blisters and bullae in the latter stages.
The patient is severely unwell in its fulminant phase, with signs and symptoms of acute septic shock and extensive organ failure. The infection is treated with broad-spectrum antibiotics initially, but early and vigorous drainage and precise debridement are the mainstays of therapy.
Besides good nutrition, postoperative wound treatment is critical for the patient's survival. With its combined advantages of continual wound washing and granulation tissue growth, the vacuum-assisted closure method has shown to be helpful in wound treatment.
Necrotizing Fasciitis Epidemiology
The yearly incidence of necrotizing fasciitis is estimated to be 500-1,000 cases yearly, with a worldwide frequency of 0.40 per 100,0,00 people. It seems to favor males, with a male-to-female ratio of 3:1; this ratio is primarily attributable to the greater prevalence of Fournier's gangrene in men.
The illness affects people of all ages, although middle-aged and elderly individuals (those over 50) are more prone to be involved. The median mortality ratio of necrotizing fasciitis is a contentious topic.
The median death rate was 21.5 percent. However, it varies widely in the literature, ranging from 8.7 to 76 percent. The mortality rate for necrotizing fasciitis of the extremities is somewhat lower than that for abdominal and perineal infections. Patients with Fournier's gangrene that has not progressed to the abdominal wall have a greater chance of survival. Without therapy, the fatality rate exceeds 100% in most cases.
Necrotizing Fasciitis Etiology
The most prevalent identified cause is trauma. Most patients had a history of minor or significant traumas, including external injuries and surgical wounds.
The most common causes of complicated intra-abdominal infections that can lead to necrotizing fasciitis are appendicitis with perforation, infection following incarcerated hernia repair, perforated diverticulitis, and necrotic cholecystitis, gastroduodenal perforation, small bowel perforation, and obstructive colon cancer with perforation.
Notably, the incidence of necrotizing fasciitis from a surgical lesion in the chest wall is higher than in comparable wounds in the lower abdomen. These patients are at a high risk of developing osteomyelitis, significantly increasing their mortality.
Fournier's gangrene is often caused by surgical incisions, abscess drainage, and pressure sores. It may also appear as a colorectal illness consequence related to anorectal infection, ischiorectal abscesses, and colon perforations.
Other probable reasons include urethral stricture and trauma from an indwelling Foley catheter. It is usually attributed to Bartholin abscesses or vulval skin infections in women.
Raw or undercooked seafood consumption and damage from fish fins may cause necrotizing fasciitis in Asia. Bacteria such as Vibriospp., Aeromonasspp., and Shewanellaspp. are typically implicated in this type of illness and are generally referred to as "marine bacteria."

Necrotizing Fasciitis
Necrotizing Fasciitis Co-Morbidities And Risk Factors
Nonsteroidal anti-inflammatory medicines (NSAIDs) or steroid treatments might reduce fever, making it challenging to diagnose necrotizing fasciitis. Diabetes mellitus affects between 40 and 60 percent of people with necrotizing fasciitis.
Cirrhosis of the liver, chronic heart failure, obesity, alcohol misuse, immunodeficiency, pre-existing hypertension, and peripheral vascular disease are all prevalent co-morbidities.
Patients with concomitant illnesses are often classified as seriously sick and need long-term intensive care. Although somewhat disputed, advanced age is another risk factor for increased incidence and death.
Necrotizing Fasciitis Pathophysiology
Because the more superficial layers (dermis and epidermis) are not damaged at first, infection develops in the hypodermis or superficial fascia. The development of necrotizing fasciitis is linked to the synergistic action of bacterial virulence factors and host-specific factors.
The synergy between the various bacteria and toxins, as well as the enzymes they create, aids in spreading infection and necrosis. Anaerobic microorganisms thrive in an anaerobic environment.
The bacterial enzymes degrade the fascia and fat are directly linked to hypodermis and superficial fascia necrosis, and the vascular origin is secondary. Invasive bacteria induce thrombosis of the nutrition arteries in the hypodermis, resulting in tissue ischemia that is exacerbated by edema.
Tissue ischemia increases infectious spread, eventually leading to skin necrosis. It also explains the typical intense pain symptoms, particularly when damaged nerve branches. Regional hypoesthesia/anesthesia is also seen in many situations.
The fascial and hypodermic necrotic spread outnumbers the skin alterations. Lymphangitis and lymphadenopathy are uncommon as a result of vascular thrombosis. Gas produced by anaerobic microorganisms may cause crepitus.
Necrotizing Fasciitis Diagnosis
The diagnosis of necrotizing fasciitis is complex, and distinguishing it from other necrotizing soft tissue diseases is much more difficult. However, the physician should do everything possible to confirm the diagnosis of necrotizing fasciitis. A delay in diagnosis may be deadly, and septic shock is unavoidable if the condition is left untreated.
- Diagnosis Using Clinical Symptoms: Local pain, swelling, and erythema are the classic signs of necrotizing fasciitis. At the infected site, tenderness, sclerosis, skin necrosis, and hemorrhagic bullae may be noticed. In the fulminant stage of the disease, the patient is critically unwell, with signs and symptoms of acute septic shock, multiple organ failure syndromes, and extensive soft tissue necrosis. The subacute form of the sickness has a slow clinical course that might last many days or weeks. Pain not proportionate to edema or erythema is the most common symptom of early necrotizing fasciitis. When clinical signs appear, the appearance resembles the late stage of necrotizing fasciitis, with visible bruises, bullae, and cutaneous necrosis caused by the necrotizing process's expansion—additional necrosis of the superficial fascia and fat results in crepitus and a thin watery malodorous discharge. Fournier's gangrene has a detailed clinical history; it often begins with perineum pain, scrotal skin irritation, and itching.
- Diagnosis Using Laboratory Tests: Certain laboratory test findings may help the clinician differentiate necrotizing fasciitis from other skin diseases, such as necrotizing soft tissue infection. A white blood cell count greater than 20,000/L is strongly predictive of necrotizing fasciitis, a common sign. Blood urea nitrogen levels larger than 18 mg/dL and serum creatinine levels greater than 1.2 mg/dL suggest that the patient is still suffering from renal failure, which is frequent in this population. The appearance of unmistakable "dishwater pus," as well as a lack of bleeding and tissue resistance to blunt finger dissection, distinguishes this illness.
- Diagnosis Using Imaging Tests: Imaging investigations may help diagnose necrotizing fasciitis. Despite its low sensitivity and specificity, plain radiography may detect gas generation in soft tissue, which is present in around half of all patients and strongly suggests Clostridium species infection. CT and MRI scans are both more sensitive and specific than standard radiography. A CT scan may reveal the extent of tissue infection, fascial edema, inflammation, and gas formation. Despite being more accurate than CT, an MRI scan is not often used due to the cost. Ultrasonography is another potential option, providing vital information regarding the kind and severity of infection, mainly when the diagnosis is uncertain. The most critical finding in diagnosis is the presence of hyperechoic foci with reverberation artifact and dirty shadowing at the site of infection, which reflects subcutaneous gas. However, ultrasonography needs a highly skilled operator, which limits its use in the intensive care unit, where patients with necrotizing fasciitis are often treated.
Necrotizing Fasciitis Microbiology
According to microbiological results, necrotizing fasciitis may be divided into four categories. The polymicrobial variety is the most frequent, accounting for 70-90 percent of cases. This infection is caused by two or more pathogens (with an average of 4.4 species), primarily seen in the trunk and perineum. In certain situations, the infection is caused by Staphylococcus aureus. Type III infections are those caused by Clostridium species or Gram-negative bacteria.
Vibrio vulnificus is a marine bacterium often isolated in Asia, while Aeromonas hydrophila may be found in freshwater, low salinity water, and soil. Type IV is caused by fungal infections, namely Candida spp. and Zygomycetes. Infections with these fungi are common following trauma; the clinical picture is aggressive and quickly spread, especially in immunocompromised individuals.
Treatment Options
The following options can be availed to treat necrotizing fasciitis:
- Treatment With Antibiotics: A polymicrobial illness should be treated with antibiotics based on its history, gram stain, and culture. For type 1 infection, anaerobic coverage is essential; effective antimicrobials include metronidazole, clindamycin, and carbapenems (imipenem). Type 2 diseases are treated with antibiotics against S. pyogenes and S. aureus, which usually coexist with the former. Comprehensive gram-negative coverage is essential for newly treated patients as initial empirical therapy. To treat type 3 necrotizing fasciitis, clindamycin and penicillin, which cover Clostridium species, should be utilized. If a Vibrio infection is discovered, it is vital to use tetracyclines and cephalosporins as quickly as possible to ensure life. Although amphotericin B or fluoroconazoles may be used to treat type 4 necrotizing fasciitis, the results are frequently disappointing. Intravenous immunoglobulin (IVIG) has been documented to neutralize critical streptococcal toxins.
- Treatment With Surgery: Surgical intervention may save a person's life and should be performed as soon as possible. A delay in treatment of more than 12 hours in fulminant necrotizing fasciitis might be fatal. Surgical debridement, necrosectomy, and fasciotomy are all critical aspects of surgical treatment. Patients with necrotizing fasciitis should be closely monitored over the next 24 hours. A "second-look operation" with intensive surgical debridement is necessary for complex surgical wounds. Necrotizing fasciitis of the abdominal wall requires special care. In the days after surgery, dressings must be changed regularly. In cases of infection progression, vigorous surgical debridement should be repeated. Hartmann's resection is considered the best treatment for diffuse peritonitis. Pressure sores, perineal abscesses, and paraplegia are all major risk factors for infection spreading to the scrotum, inguinal region, and lower abdominal wall. An orchiectomy, cystostomy, or diverting colostomy is often required. Amputation is often seen as a less intrusive therapy that results in less blood loss than radical debridement. Patients suffering from hypotension or shock benefit from amputation since they cannot bear future extensive procedures.
- Treatment With Vacuum-Assisted Closure Device: Several surgeons have started using vacuum-assisted closure (VAC) therapy for rapid and effective wound closure. A vacuum-assisted closure device is a sterile, open-cell foam sponge put into the wound and tailored to fit. This is covered with a transparent adhesive drape to create an airtight environment. The sponge is connected to a portable vacuum pump through non-collapsible tubing. The pump uses continual negative pressure to expel the sponge. The vacuum-assisted closure device's microstrain improves wound healing. Several randomized controlled studies have shown that full-thickness wounds treated using vacuum-assisted closure devices heal quicker and have a smaller wound surface area than normal gauze therapy. The most noticeable benefits of vacuum-assisted closure therapy in wound care are wound area reduction and granulation tissue formation. Other advantages, such as efficient wound cleaning and exudate clearance, make vacuum-assisted closure a potential adjunct therapy for wound closure.
People Also Ask
What Part Of The Body Does Necrotizing Fasciitis Affect?
Necrotizing fasciitis is a dangerous infection of the skin, subcutaneous tissue, and the tissue that surrounds internal organs (fascia). A variety of microorganisms causes necrotizing fasciitis, and the illness may appear abruptly and spread swiftly.
Is Necrotizing Fasciitis Curable?
Necrotizing fasciitis is a condition that can be cured. Few uncommon bacterial strains may cause necrotizing fasciitis, but since these infections spread quickly, the sooner one receives medical attention, the higher the odds of survival.
What Is The Most Common Cause Of Necrotizing Fasciitis?
Several microorganisms may cause necrotizing fasciitis, sometimes called "flesh-eating sickness." According to public health authorities, the most prevalent cause of necrotizing fasciitis is group A Streptococcus (group A strep).
How Long Can You Live With Necrotizing Fasciitis?
The average lifespan was 10.0 years (95 percent confidence interval: 7.25-13.11). Women had a greater death rate than males. Infectious diseases were responsible for 12 of the 87 fatalities.
Who Is At Risk For Necrotizing Fasciitis?
Diabetes mellitus, intravenous drug misuse, age more than 50, hypertension, and malnutrition/obesity were risk factors for necrotizing fasciitis in 25 consecutive cases.
Where Is Necrotizing Fasciitis Most Commonly Found?
The extremities are the most prevalent body regions where necrotizing fasciitis occurs (arms, hands, feet, and legs). However, necrotizing fasciitis may also develop in the head, neck, and groin areas depending on the conditions and risk factors.
Conclusion
Necrotizing fasciitis is an uncommon but deadly illness with a high mortality rate that exceeds 100% without treatment. The diagnosis of necrotizing fasciitis is complex, as is the distinction between necrotizing fasciitis and other necrotizing soft tissue infections. Antibiotic therapy has a poor value in necrotizing fasciitis, and early and forceful drainage and debridement are essential. The doctor should consider amputating the infected limb in necrotizing fasciitis of the extremities. However, this will not lessen the risk of death.

Katharine Tate
Author

Karan Emery
Reviewer
Latest Articles
Popular Articles